Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
Barth Olin
Caricato da
Nayan MaharjanCopyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
Barth Olin
Caricato da
Nayan MaharjanCopyright:
Formati disponibili
HISTORY Ms. T.T.
, 28 year-old, married, office clerk residing in Angeles City, was admitted at ER AUFMC because of labor pains. Source and Reliability: The patient herself; seems reliable. CHIEF COMPLAINT: Labor pains HISTORY OF PRESENT ILLNESS Condition started about five hours prior to admission as lumbosacral pains, regular in intensity and duration, accompanied with watery-bloody vaginal discharge. Found to be in active labor hence admitted. PAST MEDICAL HISTORY Childhood illnesses: Unremarkable Adult illnesses: Unremarkable Medical: None Surgical: None Medications: No maintenance medications Obstetric/Gynecologic: Menarche: 12 years old, lasting for 5 days, moderate in amount, no accompanying pains. Regular monthly menses, 5-7 days duration, moderate in amount, no accompanying pains. LMP- Cannot recall G1 P0 FAMILY HISTORY The patients mother is hypertensive. REVIEW OF SYSTEMS General: No easy fatigability. No weight loss. No decrease in her appetite. Skin: No rashes or other changes. Head, Eyes, Ears, Nose, Throat (HEENT) Head: No history of head injury, headache, dizziness and lightheadedness.
Eyes: No abnormal vision, wearing of eyeglasses or contact lens, pain, eye irritation, redness, excessive tearing, double vision, blurring of vision, spots, specks, glaucoma or cataracts. Ears: No abnormal hearing, earache, tinnitus, vertigo, infection, discharge, decreased hearing. Nose, sinuses: No frequent colds, nasal stuffiness, discharge, itching, hay fever, frequent nosebleeds, and sinus congestion. Throat, mouth and pharynx: No sore tongue, dry mouth or difficulty swallowing. Neck: No lumps, goiter, pain. No swollen glands. Breasts: No lumps, pain, discharge. Respiratory: No cough, hemoptysis, pleurisy, dyspnea and wheezing. Cardiovascular: No dyspnea or orthopnea, No chest pain. No palpitations. Gastrointestinal: No heartburn, vomiting, and changes in bowel habit, hemorrhoids, constipation, abdominal pain, food intolerance, and gallbladder problem. Urinary: No urinary tract infection, dysuria, hematuria, kidney stones, flank pain and incontinence. Peripheral Vascular: No intermittent claudication, frequent leg cramps and history of clots in the veins. Musculoskeletal: No arthritis, joint stiffness. Neurologic: No fainting, seizures, motor or sensory loss. She has good memory. Hematologic: No easy bleeding. Endocrine: No known thyroid trouble, temperature intolerance. Psychiatric: No history of nervousness, depression, memory loss or suicidal attempts.
PHYSICAL EXAMINATION General: The patient is conscious, coherent, and aware of the time and place, ambulatory, not in distress. Vital signs: Temperature: 36.9oC PR: 80/min BP: 120/80 mmHg RR: 18/min
Head, Eyes, Ears, Nose, Throat (HEENT)
Slightly pale conjunctivae. Others unremarkable. Thorax/Lungs: Clear breath sounds. No rales. Cardiovascular: Regular in rate and rhythm. Abdomen: Globularly enlarged, uterus contracting, FH 28cm, FHT- 138/min LLQ Musculoskeletal/ Extremities: No edema. External genitalia: No abnormalities noted Pelvic exam: Speculum exam: Vulvar wall is pinkish in color, no ulcers, and no erosions. Slight foul smelling discharge, amber in color Internal exam: Cervix BOW : 50% effaced, dilated 5cm, non-tender : intact
Cephalic presentation Bloody mucoid discharge COURSE IN THE WARD Upon admission she was brought to the labor room for monitoring. After 6 hours, she gave birth to an alive baby boy weighing 7.8 lbs, by vagina delivery after doing a left medio-lateral episiotomy. Placenta was expelled out spontaneously after 5 minutes. Local pudendal block anesthesia was given and episiotomy was repaired successfully. Uterus was contracted and vaginal bleeding was minimal, so she was brought to her room. Follow-up at her room, BP was 112/72; PR. 80/min. vaginal pad was slight soaked and uterus is wellcontracted at level of navel. BP and PR were taken every 30 minutes and were found to be constant but after 3 hours the BP was found to be going down; uterus is contracted, vaginal bleeding was minimal. Until a time came that the BP went to 60/0 and PR was 90/min. I.E. showed that there was a tender mass at the upper left vaginal vault; vaginal bleeding was minimal; uterus was well- contracted; adnexae were negative. SALIENT FEATURES This is a 28-year-old woman, G1P1, who had a spontaneous vaginal delivery over a midline episiotomy following a prolonged second stage of labor. She also manifested clinical signs of hypovolemia with BP of 60/ O mmhg despite a firm fundus and presence of minimal vaginal bleeding.
OBJECTIVE FINDINGS 28 years old Was in active labor eventually leading to vaginal delivery single uterine pregnancy ,Nullipara, Episiotomy was done Follow up BP after delivery from 112/72 down to 60/0 Tender mass at the upper left vaginal vault Uterus well-contracted Minimal vaginal bleeding Adnexae were negative PERTINENT NEGATIVES (-) abdominal distention (-) swelling identified on high rectal exam (-)report back pain, fullness or pressure in the rectoanal area, or an urge to push, or they complain of dizziness (-)bulging flanks, and a bluish discoloration in the region of the flank DIFFERENTIALS 1. Bartholins Gland Cyst A Bartholin's gland cyst is a swollen fluid-filled lump that develops from a blockage of one of the Bartholin's glands, which are small glands located on each side of the opening to the vagina. RULE IN RULE OUT Lump in the vulvar area (+) bleeding, hypotension Commonly found in women of Bartholins cyst is slow growing (Lump/ reproductive age ( especially between 20mass was discovered few hours after 29 y/o) giving birth via NSD which is suggestive of an intraoperative trauma. Usually unilateral In the face of antecedent trauma, such as after vaginal delivery, the differential diagnosis is limited to only the diagnosis of vulvar hematoma. The clinical presentation is classic. Rarely, there will not be a history of antecedent trauma, yet the clinical picture appears to be consistent with a hematoma. In such instance, consideration should be given to a coagulopathy such as von Willebrand disease, which may be associated with a spontaneous hematoma secondary to minimal trauma associated with routine daily activities. An expanding mass in the vulva without a history of trauma should also result in consideration of a Bartholin cyst (or abscess), lipoma, hemangioma, or canal of Nuck cyst. 2. Bartholin Abscess
The Bartholin duct averages approximately 2.5 cm in length. Obstruction of the ductal system of the Bartholin gland results in dilation of the duct and formation of one or more cysts. An obstructed, infected gland may form an abscess. Cyst and abscess formation of the Bartholin gland will account for the majority of symptomatic vulvar cysts observed in gynecologic practice. Rule In Tender mass at the upper left vaginal vault Rule Out Location: 4 and 8 oclock of the labia majora, classically crosses the labia minora Presence of antecedent trauma Absence of fever
3. Broad Ligament Hematoma Broad ligament hematoma results from a tear in the upper vagina, cervix, or uterus that extends into uterine or vaginal arteries.
RULE IN Most commonly following operative delivery, trauma, or surgery, but it may also occur following spontaneous vaginal delivery. Minimal bleeding Hypotension
RULE OUT (-) abdominal distention (-) swelling identified on high rectal exam (-)report back pain, fullness or pressure in the rectoanal area, or an urge to push, or they complain of dizziness Cannot totally rule out, need for imaging studies
4. Hidden vaginal or cervical lacerations Continuing hemorrhage in a patient with a firm uterine fundus may indicate a hidden vaginal or cervical laceration. "Trauma": Trauma to the uterus, cervix, and/or vagina is the second most frequent cause of postpartum hemorrhage. Injury to these tissues during or after delivery can cause significant bleeding because of their increased vascularity during pregnancy. Vaginal trauma is most common with surgical or assisted vaginal deliveries. It also occurs more frequently with deliveries that involve a large fetus, manual exploration, instrumentation, a fetal hand presenting with the head, or spontaneously from friction between mucosal tissue and the fetus during delivery.
RULE IN Most commonly following operative delivery, trauma, or surgery, but it may also occur following spontaneous vaginal delivery. Episiotomy Hypotension Firm uterine fundus
RULE OUT (-) abdominal distention Minimal bleeding No Delivery of a large infant No history of Any instrumentation or intrauterine manipulation (eg, forceps, vacuum, manual removal of retained placental fragments)
5. Retroperitoneal Hematoma RULE IN Most commonly following operative delivery, trauma, or surgery, but it may also occur following spontaneous vaginal delivery. Minimal bleeding Hypotension RULE OUT (-) abdominal distention (-) swelling identified on high rectal exam (-)bulging flanks, and a bluish discoloration in the region of the flank that appears 24 to 48 hours after a severe retroperitoneal bleed. (-)report back pain Cannot totally rule out, imaging studies needed
6. Vulval And Vulvovaginal Hematoma RULE IN Most commonly following operative delivery, trauma, or surgery, but it may also occur following spontaneous vaginal delivery. Minimal bleeding Hypotension 28 years old Was in active labor eventually leading to vaginal delivery Episiotomy was done Follow up BP after delivery from 112/72 down to 60/0 Tender mass at the upper left vaginal vault Uterus well-contracted Minimal vaginal bleeding RULE OUT No Severe vulvar or perineal pain No reports of Vaginal pressure Cannot totally rule out imaging studies needed
Adnexae were negative
Most likely diagnosis: Puerperal Vulvovaginal Hematoma to r/o Retroperitoneal hematoma and Broad Ligament Hematoma Next step: Thorough examination (including vaginal and rectal examination and possible evaluation of the uterine cavity) to evaluate for sources of blood loss and pain. Definition Postoperative Hematoma is basically a localized collection of blood outside of blood vessels in the surgery site , prompting blood to seep out of the blood vessel into the surrounding tissues. It develops just a few hours after the surgery, due to some kind of damage to the wall of the surrounding blood vessels (artery, vein, or small capillary) or as a result of poor aftercare of the patient. A hematoma usually describes bleeding which has more or less clotted, whereas a hemorrhage signifies active, ongoing bleeding. Hematomas may occur in the potential pelvic extraperitoneal spaces, including the perivaginal space, pericervical space, presacral space, and broad ligament space, and may extend superiorly to contiguous abdominal extra peritoneal spaces
INCIDENCE Puerperal hematomas are serious obstetric complications. It occurs in approximately 1 in 500 to 1 in 1500 deliveries. It occurs in approximately 1 in 1000 surgical intervention. Women At Increased Risk The pregnant uterus, vagina, and vulva have rich vascular supplies that are at risk of trauma during the birth process, and trauma may result in formation of a hematoma Women at increased risk include those who are - nulliparous, - maternal age more 29 years, - who have an infant over 4000 grams, - Preeclampsia, - prolonged second stage of labor, - instrumental delivery, - multifetal pregnancy, - vulvar varicosities, or
- clotting disorders. In cases of placenta accreta or increta, the uterus may invade other organs, making immediate surgery difficult, if not impossible. Under such circumstances, abnormal vascularity may be evident.
Clotting disorder -Hours to days after delivery, the deposition of fibrin (within the vessels in the area where the placenta adhered to the uterine wall and/or at cesarean delivery incision sites) plays a more prominent role. In this delayed period, coagulation abnormalities can cause postpartum hemorrhage alone or contribute to bleeding from other causes, most notably trauma. These abnormalities may be preexistent or acquired during pregnancy, delivery, or the postpartum period. Potential causes include the following: Platelet dysfunction: Thrombocytopenia may be related to preexisting disease, such as idiopathic thrombocytopenic purpura (ITP) or, less commonly, functional platelet abnormalities. Platelet dysfunction can also be acquired secondary to HELLP syndrome (hemolysis, elevated liver enzymes, and low platelet count). Inherited coagulopathy: Preexisting abnormalities of the clotting system, as factor X deficiency or familial hypofibrinogenemia Use of anticoagulants: This is an iatrogenic coagulopathy from the use of heparin, enoxaparin, aspirin, or postpartum warfarin. Disseminated intravascular coagulation (DIC): This can occur, such as from sepsis, placental abruption, amniotic fluid embolism, HELLP syndrome, or intrauterine fetal demise. Dilutional coagulopathy: Large blood loss, or large volume resuscitation with crystalloid and/or packed red blood cells (PRBCs), can cause a dilutional coagulopathy and worsen hemorrhage from other causes. Physiologic factors: These factors may develop during the hemorrhage such as hypocalcemia, hypothermia, and acidemia.
ANATOMY AND BLOOD SUPPLY OF FEMALE GENITAL TRACT
TYPES OF PUERPERAL HEMATOMA Superfacial wound hematoma A swollen lump under the skin near the surgery wound . It is a collection of blood and clot in the wound, is one of the most common wound complications and is almost always caused by imperfect hemostasis. The risk is much higher in patients who have been given systemically effective doses of anticoagulants and those with preexisting coagulopathies. Vigorous coughing or marked arterial hypertension immediately after surgery may contribute to the formation of a wound hematoma. Dehiscence is rare in patients under age 30 It is more common in patients with diabetes mellitus, uremia, immuno-suppression, jaundice, sepsis,
hypoalbuminemia, and cancer; in obese patients; and in those receiving corticosteroids. This is the single most important factor. The fascial layers give strength to a closure, and when fascia disrupts, the wound separates. Accurate approximation of anatomic layers is essential for adequate wound closure. Rectus Sheath Hematoma (RSH) Rectus sheath hematoma (RSH) is an uncommon and often misdiagnosed condition and an unusual cause of a painful abdominal mass. The most frequent location is infraumbilical It is the result of bleeding into the rectus sheath from damage to the superior or inferior epigastric arteries or their branches or from a direct tear of the rectus muscle. The emergency physician should be familiar with rectus sheath hematoma because it can mimic almost any abdominal condition. While usually a self-limiting entity, rectus sheath hematoma can cause hypovolemic shock following sufficient expansion, with associated mortality With early diagnosis and conservative management, surgical intervention can be avoided even with large hematomas Spontaneous resolution of RSH, especially in large hematoma, however, takes place over several months. Surgical intervention would be indicated primarily in cases in which homodynamic stability is not achieved Hematomas above the arcuate line are generally caused by damage to the superior epigastric artery or its perforating branches. Patients usually present with unilateral, small, spindle-shaped masses because these hematomas are isolated by the rectus sheath and the tendinous inscriptions, causing tamponade of the bleeding. hematomas resolve by themselves within 1 month Hematomas below the arcuate line are caused by damage to the inferior epigastric artery or its perforating branches. They protrude posteriorly and appear spherical because the rectus abdominis muscle is only supported posteriorly by the transversalis fascia and the parietal peritoneum. Below the arcuate line, hematomas bleed more and may dissect extensively because no posterior sheath wall or tendinous inscriptions are present to tamponade the bleeding. Rectus sheath hematomas below the arcuate line are more likely to cross the midline and become bilobar. hematomas usually resolve within 2-4 months. Hematomas near the umbilicus are rare. They are small when they do occur because the microscopic anastomoses of the superior and inferior epigastric arteries near the umbilicus do not allow for significant bleeding. Hematomas near the peritoneum can result in peritoneal irritation, subsequent abdominal rigidity, and gastrointestinal symptoms. Dissection of the hematoma inferiorly into the prevesicular space of Retzius can masquerade as a pelvic tumor or irritate the bladder, resulting in urinary complications SubFacial Hematoma Subfascial hematoma is an important complication of cesarean delivery. It results from extraperitoneal hemorrhage within the prevesical space, posterior to the rectus muscles
and transversalis fascia but anterior to the peritoneum and umbilicovesical fascia. Subfascial hematomas were found in 38% of patients referred for sonographic evaluation of a fever or a fall in hemoglobin that occurred after a cesarean delivery. In all cases, sonography revealed cystic or complex masses of various sizes anterior to the bladder. Some patients had concomitant bladder-flap hematomas between the lower uterine segment and posterior bladder margin. The presence of subfascial hematomas should be specifically sought in the evaluation of a febrile post cesarean patient.
Prevesical Or Retzius Space Hematoma Hematoma in Retzius' space and the anterior wall of the bladder, The venous load in the pelvic vascular system is increased during pregnancy; a stress-induced increase in venous blood pressure might play a prominent role, especially in cases of venous ectasia, where the resistance of blood vessel walls is reduced. Intraoperative evidence seemed to suggest a haemorrhage secondary to the rupture of the venous vessels in the Santorini plexus. The rupture was probably caused by the thrust of the fetal head, associated with abnormality or fragility of the blood vessels, or by some pathologic changes occurring in the anatomical structures during pregnancy, which could not be accurately defined because of the severity and degree of the hematoma infiltration found intraoperatively. In the postpartum period, the patient complained of urinary retention and pain in the hypogastric region Bladder Flap Hematoma (BFH) The bladder-flap hematoma (BFH) is an unusual complication of the cesarean section (CS) performed without peritoneal closure. It is an usual event after the visceral peritoneal closure performed during the traditional CS method. A BFH is generally thought of as a blood collection located in a space placed between the posterior bladder wall and anterior wall of lower uterine segment (LUS), vescico-uterine space. If, during a Stark CS, pathological fluid collections arise in this space by uterine suture bleeding, these decant into the large peritoneal cavity causing a hemoperitoneum. This last complication can be easily and accurately detectable by ultrasonography, which can be utilised by non-invasive monitoring as a guide for the clinical follow-up. Significant bladder-flap hematomas were characteristically round, greater than 2 cm masses asymmetrically placed in or adjacent to the uterine incision. Gas within the hematoma strongly suggests an infected hematoma.
Uterine Wound Hematoma Hematoma represents the second-most common Cesarean wound complication, occurring after
approximately 1.2 percent of deliveries. Using sonography, the incision site was visualized as an oval symmetric region of distinct echogenicity interposed between the lower uterine segment and the posterior wall of the urinary bladder. Sometimes in asymptomatic patients, a small (less than 1.5 cm) round hypoechoic mass was present in or adjacent to the uterine incision and distinct from the normal incision. These probably represented insignificant hematomas. Intramural Uterine Hematoma Couvelaire uterus - Extravasation of blood into the uterine musculature and beneath the uterine peritoneum in association with severe forms of abruptio placentae. A pseudoaneurysm of uterine artery is an extraluminal collection of blood with turbulent flow that communicates with flowing arterial blood through a defect in the arterial wall, transabdominal ultrasonography and magnetic resonance imaging revealed an intramyometrial hematoma in anterofundal region of uterus. Patient is complaining of a severe lower abdominal pain. . Intrauterine Hematoma The content of the endometrial cavity was variable in amount and appearance. The presence of retained fluid: blood or lochias (blood in 64% of cases). It was larger in the inferior uterine segment. The presence of heterogeneous echo is consistent with blood products of different ages. Endometrial fluid usually resolves after 1 week. There may only be little fluid even on early post-partum scans. Areas of hypointensity may correspond to air. Air bubbles often are visible. Air in the endometrial cavity has been described in 25% of patients following vaginal delivery and 50% of patients following C-section. Broad Ligament Hematoma Broad ligament hematoma results from a tear in the upper vagina, cervix, or uterus that extends into uterine or vaginal arteries. Most commonly following operative delivery, trauma, or surgery, but it may also occur following spontaneous vaginal delivery. These can be dangerous as they may be silent and not cause obvious vaginal bleeding. Most patients report back pain, fullness or pressure in the rectoanal area, or an urge to push, or they complain of dizziness and eventually may become hypotensive and anemic. Broad ligament hematoma may be treated either conservatively with blood transfusion, fluid resuscitation, and observation or with surgical exploration and evacuation. Or it was successfully treated by uterine artery embolization Retroperitoneal Hematoma They are potentially life-threatening conditions.
The patient may complain of intense flank pain or back pain. The patient may develop tachycardia and hypotension if the rate of hemorrhage is rapid. Rarely, later in the course, the patient may has bulging flanks, and a bluish discoloration in the region of the flank that appears 24 to 48 hours after a severe retroperitoneal bleed. Supravaginal Hematoma Supravaginal or subperitoneal. These are the result of damage to the uterine artery branches in the broad ligament. The hematoma can dissect retroperitoneally or develop within the broad ligament. It can be clinically occult despite significant blood loss. A high index of suspicion is required to diagnose and manage these hematomas promptly before signs of cardiovascular collapse develop. Vaginal Hematoma Vaginal or Paravaginal hematomas arise from damage to the descending branch of the uterine artery. The hematoma is confined to the paravaginal tissues in the space bounded inferiorly by the pelvic diaphragm and superiorly by the cardinal ligament. Rectal pain, vague lower abdominal pain but hematoma will not be obvious externally but can be diagnosed by vaginal examination. The mass often occludes the vaginal canal and extends into the ischiorectal fossa. Vulval And Vulvovaginal Hematoma In vulval hematomas bleeding is limited to the vulval tissues superficial to the anterior urogenital diaphragm. The hematoma will be evident on the vulva. Vulvovaginal hematomas are also evident on the vulva but they extend into the paravaginal tissues. Both types arise from injury to the branches of the pudendal artery (the posterior rectal, transverse perineal and posterior labial arteries). Visible hematomas that are less than 4 cm in size and not expanding may be managed with ice packs and observation. Larger or expanding hematomas must be incised, irrigated and packed, with ligation of any obvious bleeding vessels Sign and Symptoms: Swelling and appearance of a mass in the genital area discoloration of the skin; visible outline of the hematoma Severe vulvar or perineal pain Vaginal pressure Inability to urinate PATHOPHYSIOLOGY
Vulvar hematomas result from injuries to branches of the pudendal artery (inferior rectal,
perineal, posterior labial, and urethral arteries; the artery of the vestibule; and the deep and dorsal arteries of the clitoris) that occur during episiotomy or from perineal lacerations. These vessels are typically located in the superficial fascia of the anterior (urogenital) or posterior pelvic triangle. The superficial compartment of the anterior triangle communicates with the subfascial space of the lower abdomen below the inguinal ligament. Extension of bleeding in the anterior triangle is limited by Colles' fascia and the urogenital diaphragm, while the anal fascia limits extension of bleeding in the posterior triangle. As a result, bleeding is directed toward the skin where the loose subcutaneous tissues afford little resistance to hematoma formation. Superficial hematomas can extend from the posterior margin of the anterior triangle (at the level of the transverse perineal muscle) anteriorly over the mons to the fusion of fascia at the inguinal ligament. Necrosis caused by pressure and rupture of the tissue surrounding the hematoma may lead to external hemorrhage Primary and Secondary Assessment Primary survey (ABCs): Perform the A irway assessment evaluating it for patency. Assess B reathing adequacy and provide supplementation with 100% oxygen as needed. Assess the C irculatory status (including peripheral pulses, heart rate, blood pressure, and a perineal examination). Support circulation to vital organs by putting the patient into the Trendelenburg position, placing at least 2 large-bore IVs, starting a rapid crystalloid infusions through both IVs, and establishing continuous vital sign monitoring to guide continued management. Secondary survey: Perform a focused physical examination (see Physical Examination). Also, consider a bedside ultrasonography (a FAST examination to look for intra-abdominal fluid and/or a pelvic ultrasound) as an adjunct to the physical examination. Laboratory Studies Complete blood count (CBC) The hemoglobin and hematocrit are helpful in estimating blood losses. However, in a patient with acute hemorrhage, several hours may pass before these levels change to reflect the blood loss and platelet count. If the white blood cell count is elevated, suspect endometritis or toxic shock syndrome. Look for thrombocytopenia. Coagulation laboratory studies: Elevations of the prothrombin time (PT), activated partial thromboplastin time (aPTT), and international normalized ratio (INR) can indicate a present or developing coagulopathy. Electrolytes: Check for complicating electrolyte derangements such as a hypocalcemia, hypokalemia, and hypomagnesemia. Use this first set as a baseline for comparison during and after fluid and/or blood resuscitation.
BUN/creatinine: These measurements can be helpful in identifying renal failure as a complication of shock. If the BUN level rises during or after resuscitation with blood products, consider red blood cell hemolysis as a complication. Type and crossmatch: Begin the process of finding appropriately matched blood for resuscitation in the event that it is needed. Fibrinogen level: Levels are normally elevated to 300-600 mg/dL in pregnancy. Normal or low values raise concerns for a consumptive coagulopathy. Liver function tests (LFTs), amylase, lipase: These studies can be helpful in considering other abdominal pathology, such as HELLP syndrome, if there is abdominal pain in addition to, or instead of, uterine tenderness. Lactate: Consider ordering this if the initial electrolyte study shows an anion gap or septic or hypovolemic shock is suspected as a concomitant diagnosis.
IMAIGING STUDIES Ultrasound, computed tomography (CT) and magnetic resonance imaging (MRI) scans will mainly be useful for diagnosing hematomas above the pelvic diaphragm and to assess any extension into the pelvis, particularly as bimanual examination may not find them until they are quite large. MRI can also be particularly useful in providing information on the location, size and extent of a hematoma and in monitoring progress or resolution. Imaging Studies Studies to be considered with vaginal bleeding and decreasing red blood cell counts in the postpartum patient include ultrasonography (U/S), computed tomography (CT), or magnetic resonance imaging (MRI). Ultrasonography is a fast and helpful modality for imaging pelvic structures and should be the first-line study for pelvic pathology. Ultrasonography In a hemodynamically unstable patient, a bedside ultrasonography can be performed by an experienced emergency medicine provider as an extension of the physical examination. In general, a dedicated pelvic ultrasonography (transabdominal and/or transvaginal) is helpful in identifying large retained placental fragments, hematomas, or other intrauterine abnormalities. Retained placenta and hematoma can look ultrasonographically identical. Using a Doppler ultrasound to look for vascularity can help to differential between the two, with clots being avascular and retained placenta often receiving persistent blood flow from the uterus.
The abdominal views of the focused assessment with sonography in trauma (FAST) examination are helpful in identifying fluid within the peritoneum that may be the result of hemorrhage. This study is designed to identify intra-abdominal and pericardial fluid that requires early operative intervention in trauma patients. However, the abdominal views are useful in any patient with suspected intraabdominal free fluid. These include views of the right upper quadrant (RUQ)/Morison's pouch area (the most dependent area of a supine patient's peritoneal cavity), the left upper quadrant (LUQ) spleno-renal recess, and views of the pelvis (sagittal and coronal views of the uterus and pouch of Douglas). This study can detect 250-500 mL of fluid in the peritoneum, but it is a poor study for identifying retroperitoneal or paravaginal hemorrhage (extra-peritoneal bleeding). Ultrasonography cannot reliably differentiate between blood, urine, or ascites; however, in the setting of suspected hemorrhage, any fluid in the abdomen should prompt further investigation. More stable patients can have their abdominal and/or pelvic ultrasonography confirmed with an official study performed by a radiologist. Computed tomography In the event that ultrasonography is not diagnostic, CT is a helpful follow-up study. This may also be the first-line study when a pelvic hematoma or abscess is suspected, which may be missed with a sonogram. The traditional teaching is that pelvic CT is a less than ideal study for pelvic structures, due to artifact from the surrounding pelvic bones that reduces the image quality. However, this is generally not the case with modern multidetector CT studies. When enhanced with intravenous (I+) and intra-intestinal (O/R+...either oral or rectal contrast), CT can detail pelvic hematomas, cesarean delivery wound dehiscence, and retained placental tissue. Magnetic resonance imaging MRI is a time consuming study that is rarely performed from the ED in these patients. It can be helpful in delineating tissue planes to determine if a fluid collection (hematoma or abscess) is intrauterine or extrauterine when this is not clear from ultrasonography or CT. It can also help to distinguish a placenta accreta from simple retained products of conception. Limited literature is available on abdominopelvic imaging in postpartum hemorrhage since the presentation of significant bleeding prompts rapid resuscitation and immediate intervention based on the clinical picture rather than documented imaging. Nonetheless, all 3 imaging modalities can assist in the evaluation of a bleeding source, but ultrasonography is usually sufficient for emergent situations. Size Of Hematoma The three main diameters of any detected echo free areas were measured (the radius was obtained by dividing this measurement by two).
The volume of the fluid collection was calculated using the formula for an ellipse (4/3 r1 r2 r3). The vaginal vault, the pouch of Douglas, the bladder flap area and the abdominal wall were systematically examined. Characteristics of the fluid collection were recorded. A parietal wall collection was defined as any subcutaneous or subfascial echo-free area. Pelvic collections were diagnosed when the volume of the echo-free area was greater than 20 Ml. Prophylactic Antibiotics One fourth of all postoperative hematomas are already contaminated. Ultrasonographical examination is an effective method for early recognition of such postoperative hematomas. Ultrasonic diagnosis on a routine basis is not necessary, but it should be carried out as soon as clinical symptoms appear. Postoperative hematoma formation must be treated as a potential infection. MANAGEMENT Short Term
Management aims to prevent further blood loss, minimize tissue damage, ease pain and reduce the risk of infection. Resuscitative measures should be considered the first line of treatment. See Imaging Studies for more detail. Interventions: Address the "4Ts plus 1" starting with "tone" since it is the most common cause of postpartum hemorrhage: then trauma, tissue and thrombocytopenia
Hematomas should not be disrupted if they are unruptured. However, steady pressure may be applied to prevent expansion. If there is no other cause of blood loss, resuscitate the patient and admit her to the hospital with a plan to monitor the hematoma for expansion and follow her hemoglobin and hematocrit levels. The extent of the blood loss is often underestimated and a high index of suspicion is required. Aggressive fluid replacement and assessment of coagulation status is essential if there is heavy bleeding or signs of hypovolaemia. Blood should be available for transfusion. Evaluate the CBC and coagulation study results for evidence of clotting disorders. Providing blood products will be necessary if the bleeding is profuse or initial laboratory results show hemoglobin drop >10% from the patient's prior value or from the midpoint of the normal range with continued bleeding. For anemia, transfuse type-specific blood (or O- blood if unable to wait). Using blood warmers that
permit rapid infusion is highly recommended as long as this does not delay transfusion. For thrombocytopenia, particularly if platelets are less than 50,000, consider transfusing a pack of platelets. Fresh frozen plasma (FFP) may also be necessary in the setting of a coagulopathy (prolonged PT or PTT or INR >1.3). In the event of massive hemorrhage, plasma transfusion should be initiated with the replacement of red blood cells to avoid a dilutional coagulopathy by adding back a proportional amount of clotting factors.[13] If transfusing more than 6 units of pRBCs occurs or is anticipated, give 4 units of FFP, 1 unit of platelets, and 1 unit of cryoprecipitate to avoid a transfusion-related dilutional coagulopathy. The effects of any anticoagulant medications that the patient may have on board should be reversed (aspirin with platelets, low molecular weight heparin [LMWH] or heparin with protamine, warfarin with vitamin K or FFP). A urinary catheter is generally advocated to monitor fluid balance and to avoid possible urinary retention resulting from pain, oedema or the pressure of a vaginal pack. Small, static hematomas (5 cm in diameter) can be managed conservatively. Conservative management of larger hematomas has been associated with longer stays in hospital, an increased need for antibiotics and blood transfusion and greater subsequent operative intervention. A hematoma that expands acutely is unlikely to settle with conservative measures more 5 cm) vulval hematomas are best managed with surgical evacuation, primary closure and compression for 1224 hours. Surgical management of larger subperitoneal hematomas requires an abdominal approach with identification and ligation of bleeding vessels, or arterial embolisation under radiological control is now an alternative. The clot should be evacuated. They can be difficult to diagnose, as symptoms can be non-specific and bleeding is often concealed. Surgical management /Operative Approach For vulvovaginal hematomas, an incision should be made of appropriate size (often 5-10 cm in length) to gain access to the hematoma. All clots should be removed and the area irrigated copiously. In most settings, a diffuse oozing tissue bed will be identified as opposed to discrete bleeding vessels which could be ligated or cauterized. A layered closure should then be performed to provide hemostasis and close dead space. A vaginal pack can be used if considered necessary; placement of the pack should be done with care to prevent disruption of the closure of the hematoma site and to avoid creation of additional bleeding sites as the vaginal mucosa is often friable and the patient may also be at risk for coagulopathy. Broad-spectrum antibiotics are indicated due to the risk of infection, and transfusion of blood products is often necessary.
The use of drains in the setting of a vulvovaginal hematoma is also not clearly established. The theoretical advantage of placement of drains include further elimination of dead space, reduction of pressure and possible resultant tissue necrosis, and removal of necrotic tissue and blood that may provide a source of infection.Varied approaches to drainage have been described, including placement of a Penrose drain brought out through the introitus and a closed system Jackson-Pratt drain exiting through a separate perineal site. JACKSON-PRATT DRAIN: A closed-system drain consisting of a flat white perforated ribbon to be placed in the bed of a hematoma cavity following evacuation of blood and clot. The ribbon connects to a short length of plastic tubing which can be exited through a separate stab wound in the perineum and connected to a hand grenade suction device. Such a drain is felt by some investigators to be an important adjunct in the management of moderate-to-large vulvovaginal hematomas. Angiographic Embolization Angiographic embolization has been described for various obstetric and gynecologic conditions, including management of postpartum hemorrhage and leiomyomatous uteri. Embolization has also been described in the management of vulvovaginal hematomas, mainly in the setting of hematomas not responsive to initial therapy.Theoretically, embolization may also be an option for management of supralevator hematomas, since embolization has been used to successfully control severe retroperitoneal bleeding in other clinical scenarios.
Long Term Management Health teachings on perineal exercises to strengthen the muscles.
POTENTIAL COMPLICATONS: Short-term: severe hemorrhage (including retroperitoneal hematoma), transfusion, coagulopathy. Long-term: infection, scarring/disfigurement, dyspareunia. PROGNOSIS The prognostic outcome of this rare case of post-partum hemorrhagia is highly dependent on early diagnosis and rapid treatment involving close cooperation between obstetricians and anesthetists, and also of rapid embolization to prevent possible intractable hematomas. CONCLUSION
Genital tract hematomas are uncommon and can cause diagnostic confusion. Clinicians must be alert to hematomas as a differential diagnosis of postpartum pain and bleeding. The most important factor in correct diagnosis is clinical awareness. Excessive perineal pain is a hallmark symptom: its presence should prompt examination. Aggressive fluid resuscitation/blood transfusion may be required. Coagulation status should be monitored. Treatment should be carried out in an operating theatre. A urinary catheter should be used to prevent urinary retention and monitor fluid balance. The threshold for using antibiotics should be low. There is no evidence to support best management, which can be primary repair or packing, with or without insertion of a drain. Vigilance should be maintained after primary repair/packing, as recurrence is common. .REFERENCES 1. Shiono PH, McNellis D, Rhoads GG. Reasons for the rising cesarean delivery rates: 19781984. Obstet Gynecol. 1987;69:696700. 2. Stanley FJ, Watson L. Trends in perinatal mortality and cerebral palsy in Western Australia, 1967 to 1985. BMJ. 1992;304:165863.
Potrebbero piacerti anche
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- NeurologicDocumento7 pagineNeurologicFarrah ErmanNessuna valutazione finora
- Attention DeficitDocumento1 paginaAttention DeficitNayan MaharjanNessuna valutazione finora
- Guia Manejo de Itu de Pediatrics 2011Documento18 pagineGuia Manejo de Itu de Pediatrics 2011Daniela CampoNessuna valutazione finora
- Anxiety Disorder - Nayan MaharjanDocumento52 pagineAnxiety Disorder - Nayan MaharjanNayan MaharjanNessuna valutazione finora
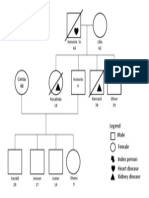
- Family GenogramDocumento1 paginaFamily GenogramNayan MaharjanNessuna valutazione finora
- Cancer Awareness Month 2013: Obstetrics and Gynecology DepartmentDocumento1 paginaCancer Awareness Month 2013: Obstetrics and Gynecology DepartmentNayan MaharjanNessuna valutazione finora
- Apple SupportDocumento1 paginaApple SupportNayan MaharjanNessuna valutazione finora
- Timetable and Proponents of The StudyDocumento4 pagineTimetable and Proponents of The StudyNayan MaharjanNessuna valutazione finora
- Examination of ChestDocumento24 pagineExamination of ChestNayan MaharjanNessuna valutazione finora
- Women WaveDocumento3 pagineWomen WaveNayan MaharjanNessuna valutazione finora
- AbnormalL Liver Function Test 2012Documento59 pagineAbnormalL Liver Function Test 2012Nayan MaharjanNessuna valutazione finora
- 2b.lens and CataractDocumento3 pagine2b.lens and CataractNayan MaharjanNessuna valutazione finora
- Diabetes MellitusDocumento55 pagineDiabetes MellitusNayan MaharjanNessuna valutazione finora
- Urinary Tract Infections, Pyelonephritis and Prostatitis2011-2012Documento27 pagineUrinary Tract Infections, Pyelonephritis and Prostatitis2011-2012Nayan MaharjanNessuna valutazione finora
- Obstructive Uropathy Case StudyDocumento19 pagineObstructive Uropathy Case StudyNayan MaharjanNessuna valutazione finora
- Traumatic Brain InjuryDocumento32 pagineTraumatic Brain InjuryNayan Maharjan100% (1)
- Ophthalmoscopy, Retina, Ocular ManifestationsDocumento10 pagineOphthalmoscopy, Retina, Ocular ManifestationsNayan MaharjanNessuna valutazione finora
- Adrenoceptor Agents (Compatibility Mode)Documento19 pagineAdrenoceptor Agents (Compatibility Mode)Nayan MaharjanNessuna valutazione finora
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (588)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (74)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2259)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (121)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- Administering MedicationsDocumento24 pagineAdministering MedicationsCharmie GandaNessuna valutazione finora
- Guía Clínica HTA 2011Documento310 pagineGuía Clínica HTA 2011marcelagarciavNessuna valutazione finora
- Mayur - 01Documento2 pagineMayur - 01mukesh jambukiyaNessuna valutazione finora
- Stereotactic Neurosurgery in The United Kingdom .23Documento14 pagineStereotactic Neurosurgery in The United Kingdom .23Pablo SosaNessuna valutazione finora
- Kainan University ApplicationDocumento25 pagineKainan University ApplicationGeraldine RiveraNessuna valutazione finora
- Prenatal DevelopmentDocumento29 paginePrenatal DevelopmentReymart MancaoNessuna valutazione finora
- York County Court Schedule For Aug. 20Documento15 pagineYork County Court Schedule For Aug. 20York Daily Record/Sunday NewsNessuna valutazione finora
- Ilovepdf Merged PDFDocumento134 pagineIlovepdf Merged PDFhelalNessuna valutazione finora
- Introduction To Homoeopathic PharmacyDocumento12 pagineIntroduction To Homoeopathic PharmacyPreethika PadmanabanNessuna valutazione finora
- ECAM2015 324369 PDFDocumento6 pagineECAM2015 324369 PDFLuiz Otavio CostaNessuna valutazione finora
- Oplan Kalusugan Sa DepEd SY 2019Documento4 pagineOplan Kalusugan Sa DepEd SY 2019Klaribelle Villaceran100% (1)
- Guide To Right Dose 03508199Documento172 pagineGuide To Right Dose 03508199Antonio GligorievskiNessuna valutazione finora
- Formation of Faeces and DefaecationDocumento15 pagineFormation of Faeces and Defaecationzurich100% (5)
- Top 50 Global Stem Cell InfluencersDocumento25 pagineTop 50 Global Stem Cell InfluencersranasoftNessuna valutazione finora
- Your Health Book - Sampler by Joseph Pilates PDFDocumento28 pagineYour Health Book - Sampler by Joseph Pilates PDFMacsim Alexandra50% (2)
- Quantitative Estimation of Phytoconstituents of Caesalpinia PulcherrimaDocumento5 pagineQuantitative Estimation of Phytoconstituents of Caesalpinia PulcherrimaSriArthiNessuna valutazione finora
- Drugs and BruxismDocumento14 pagineDrugs and BruxismAnthony HartonoNessuna valutazione finora
- Advanced Trauma Life Support (Atls)Documento44 pagineAdvanced Trauma Life Support (Atls)Danar Syahrial PradhiptaNessuna valutazione finora
- KJO2086Documento13 pagineKJO2086jieunNessuna valutazione finora
- Neutral Zone Concept and Its Technique at Impression Stage PDFDocumento7 pagineNeutral Zone Concept and Its Technique at Impression Stage PDFgeneral generalNessuna valutazione finora
- Inborn Error of MetabolismDocumento33 pagineInborn Error of MetabolismAlmiraNessuna valutazione finora
- Dealing With PatientDocumento14 pagineDealing With PatientAnggih PriyantoNessuna valutazione finora
- Dafpus IugrDocumento2 pagineDafpus IugrannisaNessuna valutazione finora
- Sothys, The Professional DifferenceDocumento29 pagineSothys, The Professional DifferenceNazihCosmeticsNessuna valutazione finora
- Fascial Manipulation Practical Part PDFDocumento2 pagineFascial Manipulation Practical Part PDFBrandi0% (1)
- Bronchogenic Carcinoma: DR Ayman El-DibDocumento40 pagineBronchogenic Carcinoma: DR Ayman El-DibMuhdZaeedNessuna valutazione finora
- The 100 Most Influential Publications in Paracetamol Poisoning TreatmentDocumento81 pagineThe 100 Most Influential Publications in Paracetamol Poisoning TreatmentPetrov MihaelaNessuna valutazione finora
- Mechanical Ventilation 2015Documento18 pagineMechanical Ventilation 2015Nauman GilaniNessuna valutazione finora
- Read The Text and Answer Questions 5 and 6.: Cookbook. New York: DK Publishing, 2007, P. 8Documento1 paginaRead The Text and Answer Questions 5 and 6.: Cookbook. New York: DK Publishing, 2007, P. 8matheus gonçalvesNessuna valutazione finora
- Ebook Atlas of Interventional Orthopedics Procedures Essential Guide For Fluoroscopy and Ultrasound Guided Procedures PDF Full Chapter PDFDocumento68 pagineEbook Atlas of Interventional Orthopedics Procedures Essential Guide For Fluoroscopy and Ultrasound Guided Procedures PDF Full Chapter PDFcharles.schmidt276100% (26)