Documenti di Didattica
Documenti di Professioni
Documenti di Cultura
KariWilliams ManagementHospitalized
Caricato da
CindyDescrizione originale:
Titolo originale
Copyright
Formati disponibili
Condividi questo documento
Condividi o incorpora il documento
Hai trovato utile questo documento?
Questo contenuto è inappropriato?
Segnala questo documentoCopyright:
Formati disponibili
KariWilliams ManagementHospitalized
Caricato da
CindyCopyright:
Formati disponibili
3/18/11
Management of the Hospitalized Patient with COPD
March 26, 2011 Focus on Respiratory Care & Sleep Medicine Conference
Jennifer S. Williams, MMS, PA-C Mayo Clinic in Arizona, Instructor in Medicine Midwestern University, Clinical Instructor Kari J. Williams, ANP-BC, ACNP-BC, RN Mayo Clinic in Arizona
Objectives
List the etiologies, signs, and symptoms of a COPD exacerbation Describe indications for hospitalization during a COPD exacerbation Discuss treatment options for the hospitalized patient with a COPD exacerbation Identify perioperative risks for the hospitalized patient with COPD Determine perioperative treatment methods for the hospitalized patient with COPD
Chronic Obstructive Pulmonary Disease
3/18/11
Chronic Obstructive Pulmonary Disease
Global Initiative for Chronic Obstructive Lung Disease (GOLD)
Chronic obstructive pulmonary disease (COPD) is a preventable and treatable disease with some significant extrapulmonary effects that may contribute to the severity in individual patients. Its pulmonary component is characterized by airflow limitation that is not fully reversible. The airflow limitation is usually progressive and associated with an abnormal inflammatory response of the lungs to noxious particles or gases."
http://www.goldcopd.org.
COPD
Chronic bronchitis
Chronic inflammation of bronchial mucous membranes characterized by chronic cough
Productive cough for 3 months in at least 2 consecutive years
Emphysema
Abnormal enlargement of distal air spaces and destruction of bronchial walls and alveoli without fibrosis http://www.prlog.org/10955996-study-links-exerciseto-stronger-breathing-muscles-for-copd.html
Etiology
Tobacco use or exposure Chemical/toxin exposure Air pollution 1-antitrypsin deficiency
http://blog.epiren.com/2009_08_01_archive.html
3/18/11
Pathophysiology
Exposure to irritant Chronic inflammation
Small airway disease Parenchymal destruction
Chronic airflow limitation
Adapated from http://www.goldcopd.org.
Pathophysiology
http://www.mayoclinic.com/health/medical/IM00989
Symptoms
Dyspnea Chronic productive cough Wheezing Chest tightness exercise capacity Fatigue Anorexia and weight loss in severe disease
3/18/11
10
Physical Examination
Hypoxia Tachypnea Shallow, pursed-lip breathing breath sounds Prolonged expiratory phase Rhonchi Wheezes Barrel-shaped chest Cyanosis Clubbing
11
Pulmonary function tests (PFTs)
Forced expiratory volume in one second (FEV1) FEV1/forced vital capacity (FVC) Diffusing capacity of the lung for CO (DLCO) Total lung capacity (TLC) Residual volumes
FEV1/FVC <70% post-bronchodilator that is not fully reversible
airflow limitation
COPD PFTs
http://www.mayoclinic.com/health/medical/IM01608
3/18/11
13
PFTs and COPD Staging
Stage 1: Mild II: Moderate III: Severe IV: Very severe FEV1/FVC <70% <70% <70% <70% FEV1 80% predicted 50% 30% FEV1 <80% predicted FEV1 < 50% predicted
FEV1 < 30% predicted or FEV1 < 50% predicted + chronic respiratory failure
Adapated from http://www.goldcopd.org.
14
COPD CXR
15
Chest Radiograph (CXR)
Findings
Hyperinflation
Diaphragm flattening retrosternal air space
AP diameter Parenchymal bullae or subpleural blebs Enlargement of central pulmonary arteries Vertical and narrow heart sillouette
Prominent right heart border
3/18/11
16
COPD CT Scan
www.uptodate.com
17
Arterial Blood Gas (ABG)
Obtain if:
Signs of respiratory failure
Hypoxemia or hypercapnia are suspected
If FEV1 < 50% predicted Clinical signs of right heart failure
18
Treatment
Tobacco cessation Inhalers and small volume nebulizers (SVNs) Glucocorticosteroids Methylxanthines Pulmonary rehabilitation Additional treatment methods
3/18/11
Tobacco Cessation
Only way to slow progression of COPD Slows the decline in FEV1 in middle-aged smokers with mild airway obstruction Ex-smokers need up to six months to recover alveloar macrophage antimicrobial function
http://hometestingblog.testcountry.com/?tag=no-smoking
20
Tobacco Cessation
5% success rate with simply telling a patient to quit Cessation methods
Nicotine transdermal patch Nicotine gum Pharmacologic agents Behavior modification
CURRENT Medical Diagnosis and Treatment. 2007
21
Inhalers and SVNs
Bronchodilators
Most important agents in pharmacologic management of COPD Improve symptoms, exercise tolerance, and overall health status
http://www.asthmaready.org/Story.aspx?storyid=20
3/18/11
22
Inhalers and SVNs
Anticholinergics
Short-acting
Ipratropium bromide (Atrovent)
Long-acting
Tiotropium (Spiriva)
23
Inhalers and SVNs
2-agonists
Short-acting
Salbutamol (Albuterol) Levalbuterol (Xopenex)
Long-acting
Salmeterol (Servent)
Short-acting
2-agonist
+ anticholinergic
Ipratropium + salbutamol (Combivent)
24
Glucocorticosteroids
Oral Inhaled
For symptomatic patients with Stage III/IV COPD or with repeated exacerbations
Beclomethasone (QVAR) Budesonide (Pulmicort) Fluticasone (Flovent)
Glucocorticosteroid + long-acting
Fluticasone/Salmeterol (Advair) Budesonide/Formoterol (Symbicort)
2-agonist
3/18/11
25
Methylxanthines
Theophylline
Use is controversial Toxicity
Dose-dependent Symptoms
Cardiac arrhythmias, seizures, headache, nausea, heartburn
26
Recommended Treatment by Stage
Risk Factors, Vaccines Short-acting bronchodilator when needed 1 longacting bronchodilator when needed; rehab Inhaled steroids if repeated exacerbations Long-term oxygen if chronic respiratory failure; consider surgery
Stage I: Mild Stage II: Moderate Stage III: Severe Stage IV: Very Severe
+ + + +
+ + + + + + + + + +
Adapated from http://www.goldcopd.org.
27
Additional Treatment
Avoidance of irritants Energy conserving techniques and pulmonary rehabilitation Influenza and pneumococcal vaccinations Supplemental oxygen Opioids Surgery
Bullectomy, lung volume reduction, lung transplantation
3/18/11
28
COPD Exacerbation
29
COPD Exacerbation
Global Initiative for Chronic Obstructive Lung Disease (GOLD)
An event in the natural course of the disease characterized by a change in the patients baseline dyspnea, cough, and/or sputum that is beyond normal day-to-day variations, is acute in onset, and may warrant a change in regular medication in a patient with underlying COPD
http://www.goldcopd.org.
30
Etiology
Viral infection
Detectable in sputum/nasal lavage in 56% of patients Most commonly Picornaviruses (36%), Influenza A (25%), and Respiratory Syncytial Virus (22%)
Bacterial infection
Chronic lower airway bacterial colonization Most commonly Haemophilus influenzae, Streptococcus pneumoniae, and Moraxella catarrhalis
Clinics in Chest Medicine. 2007
10
3/18/11
31
Etiology
Environmental pollution
Particulate matter from diesel exhaust
Changes in environmental temperature Worsening of underlying comorbid conditions (HF/CKD) can precipitate an exacerbation Often, a clear precipitant is not apparent.
32
Pathophysiology
Expiratory flow limitation with mucus production, airway edema, and bronchoconstriction end-expiratory volume with dynamic hyperinflation Impairment of respiratory muscles Dyspnea, tachypnea, and difficulty of muscles to cope with respiratory demand
33
Symptoms
Increased:
Dyspnea (64%) Sputum purulence (42%) Sputum volume (26%) Wheeze (35%) Nasal symptoms (35%) Cough (20%) Mental status change
Clinics in Chest Medicine. 2007
11
3/18/11
34
CXR
CT Scan
36
ABG
Findings
Compensated respiratory acidosis with worsening acidemia Serial ABGs Comparison to baseline PaO2 <60 mmHg and/or SaO2 <90% with or without PaCO2 >50 mmHg when breathing room air respiratory failure
12
3/18/11
37
Diagnostic Studies
Sputum culture
Streptococcus pneumoniae Haemophilus influenzae Moraxella catarrhalis
PFTs
Not recommended
Influenza screening CBC and BMP ECG
38
Indications for Hospitalization
Marked in intensity of symptoms Severe underlying COPD at baseline Onset of new physical signs
Cyanosis, peripheral edema
Failure to respond to initial medical management Significant comorbidities Frequent exacerbations Newly occurring arrhythmias Older age Insufficient home support
http://www.goldcopd.org.
Indications for ICU Admission
Severe dyspnea that responds inadequately to initial emergency therapy Changes in mental status Persistent or worsening hypoxemia (PaO2 <40 mmHg) and/or severe/worsening hypercapnia (PaCO2 >60 mmHg) and/or severe/worsening respiratory acidosis (pH <7.25) despite supplemental oxygen and noninvasive ventilation Need for invasive mechanical ventilation Hemodynamic instability
http://www.goldcopd.org.
13
3/18/11
40
The Hospitalized COPD Patient
10% in-hospital mortality rate
25% require ICU admission
24% mortality rate if admitted to the ICU
More commonly admitted in the winter months
50% more common at this time due to illnesses in viral
Chest. 2008
41
Treatment
Tobacco cessation Oxygen Inhalers and small volume nebulizers (SVNs) Glucocorticosteroids Antibiotics Non-invasive positive pressure ventilation (NIPPV) Invasive mechanical ventilation
Oxygen
Goal To prevent acidosis and tissue hypoxia
PaO2 >60 mmHg SaO2 > 90%
Watch for CO2 retention
14
3/18/11
43
Inhalers and SVNs
Bronchodilators
Short-acting
2-agonists*
Salbutamol (Albuterol) Levalbuterol (Xopenex)
Anti-cholinergic
Ipratropium bromide (Atrovent) Tiotropium (Spiriva)
Significantly improve the FEV-1 Additive effect when used in conjunction with each other
44
Glucocorticosteroids
Associated with improved lung function, length of hospitalization, and in treatment failure PO vs. IV
Low-dose oral steroids were not associated with worse outcomes than high-dose intravenous therapy.
JAMA. 2010
45
Antibiotics
Indications
Symptoms suggestive of an underlying infectious etiology
dyspnea, sputum volume, and sputum purulence sputum purulence + dyspnea or sputum volume
Severe exacerbation, requiring mechanical ventilation
Invasive or non-invasive
15
3/18/11
46
Antibiotics
Choice of antibiotic and duration of treatment depend on the severity of the exacerbation
First line
Amoxil (Amoxicillin) Doxycycline Trimethoprim/Sulfamethoxazole (Bactrim)
Second line
2nd and 3rd generation cephalosporins Flouroquinolones
Antibiotics
Consider Gram-negative bacilli and Pseudomonas aeruginosa in the following patients:
Severe COPD at baseline Elderly Receiving multiple or frequent antibiotics Requiring mechanical ventilation Recent hospitalization Are more susceptible to resistant pathogens
48
The Evidence
Compared to placebo:
Systemic glucocorticosteroids
treatment failure by 46% length of hospital stay by 1.4 days FEV1 by 0.13 L three days after therapy
Antibiotics
treatment failure by 46% in-hospital mortality by 78%
Chest. 2008
16
3/18/11
49
NIPPV
BiPAP and CPAP High-flow oxygen Advantages
need for endotracheal intubation length of hospitalization mortality
http://emedicine.medscape.com/article/304235-overview
NIPPV
Indications
Moderate to severe dyspnea with the use of accessory muscles/paradoxic abdominal motion Moderate to severe acidemia (pH < 7.35) and/or hypercapnia (PaCO2 > 45 mm Hg) Respiratory rate > 25 breaths per minute
http://www.goldcopd.org.
51
NIPPV
Contraindications
Respiratory arrest CV instability
Hypotension, MI, arrhythmias
Diminished mental status Inability or unwillingness of patient High aspiration risk Copious secretions Extreme obesity Recent facial/gastroesophageal surgery Craniofacial trauma
http://www.goldcopd.org.
17
3/18/11
52
The Evidence
Compared to standard therapy
NIPPV
risk of intubation by 65% in-hospital mortality by 55% length of hospital stay by 1.9 days
Chest. 2008
Discharge Criteria
Inhaled
2-agonist therapy Q4 hours Ambulation without significant symptoms Clinical stability for 12-24 hours Appropriate home and follow-up arrangements Patient understanding of outpatient treatment plan
54
Preventing Future Exacerbations
Tobacco cessation Self-management education Vaccinations Pulmonary rehabilitation ? prophylactic antibiotics
18
3/18/11
55
Perioperative Management of Patients with COPD
Surgical Complications
Cardiac Pulmonary
Pneumonia Atelectasis airflow obstruction COPD exacerbation risk of acute respiratory failure
Considerations
COPD severity Tobacco use Age >60 Obesity Heart failure Poor general health status/performance status
Thorough history and physical examination needed to identify risk factors
19
3/18/11
Factors Associated with Increased Risk
Type of surgery
Abdominal, thoracic, vascular, head and neck, neurosurgery, emergency surgery
Surgical site
risk as incision approaches diaphragm
Length of surgery
Prolonged surgery (>3 hours)
Anesthesia
General > epidural or spinal
Preoperative Interventions
Tobacco cessation
Moller et al (2002): Hip and knee replacements
Cessation 6-8 weeks preoperatively postoperative morbidity
Wein (2009): CABG
Cessation weeks prior have risk of postoperative respiratory complications
Due to transient in sputum production
Improves wound healing
Preoperative Interventions
CXR PFTs
Not routinely recommended
But recommended prior to lung resection
ABG
Recommended prior to lung resection
20
3/18/11
61
Preoperative Interventions
Patients with symptomatic COPD should receive daily inhaled ipratropium or tiotropium prior to surgery. Patient education
Lung expansion maneuvers
Preparation is key!
incidence of pulmonary complications in those receiving preoperative preparation
Combination of bronchodilators, antibiotics, and glucocorticosteroids if necessary
When to Proceed
If COPD exacerbation is present, do not proceed with surgical procedure. If COPD stable, treat with traditional treatment modalities.
Postoperative Interventions
Lung expansion modalities
Incentive spirometer Cough and deep breathing risk of pulmonary complications by Chest percussion Suctioning Early ambulation Intermittent positive-pressure breathing
Can cause abdominal distention
NIPPV
http://healthpages.org/wp-content/uploads/2010/06/ incentive-spirometer-300x300.jpg
21
3/18/11
64
Postoperative interventions
Pain control
Leads to earlier ambulation Improves ability to breathe deeply Epidural analgesia vs. opioids
Use of nasogastric tube as needed
risk of atelectasis and pneumonia
65
Postoperative Interventions
Inhaled beta-agonists
As needed for symptomatic wheezing
Glucocorticosteroids
Persistent wheezing/functional limitations despite bronchodilator therapy
66
References
Ali, NK. Evidence-based approach to acute exacerbations of chronic obstructive pulmonary disease. Hospital Physician. 2009; 38: 9-16. From the Global Strategy for the Diagnosis, Management and Prevention of COPD, Global Initiative for Chronic Obstructive Lung Disease (GOLD) 2010. Available from: http://www.goldcopd.org. Hurst JR, Wedzicha JA. The biology of a chronic obstructive pulmonary disease exacerbation. Clinics in Chest Medicine. 2007; 28: 525-536. Lindenauer PK, Pekow PS, Lahti MC, Lee Y, et al. Association of corticosteroid dose and route of administration with risk of treatment failure in acute exacerbation of chronic obstructive pulmonary disease. JAMA. 2010; 303(23): 2359-2367.
22
3/18/11
67
References
Moller AM, Villebro N, Pedersen T, Tonneson H. Effect of preoperative smoking intervention on postoperative complications: a randomised clinical trial. Lancet. 2002; 359: 114-117. Papadakis MA, McPhee SJ. Current Consult Medicine. New York, NY: McGraw Hill Lange; 2007. Papadakis MA, McPhee SJ, Tierney LM. CURRENT Medical Diagnosis and Treatment. McGraw Hill Lange; 2007. Poon CA, Becker, KA, Littner, MR. Noninvasive positive airway pressure in hypercapnic respiratory failure in noncardiac medical disorders. Sleep Medicine Clinics. 2010; 5: 451-470.
68
References
Qaseem A, Snow V, Fitterman N, Hornbake ER, et al. Risk assessment for and strategies to reduce perioperative pulmonary complications for patients undergoing noncardiothoracic surgery: a guideline from the American College of Physicians. Annals of Internal Medicine. 2006; 144(8): 575-581. Quon BS, Gan WQ, Sin DD. Contemporary management of acute exacerbations of COPD: a systematic review and metanalysis. Chest. 2008; 133: 756-766. Wien RO. Preoperative smoking cessation: impact on perioperative and long-term complications. Arch Otolaryngol Head Neck Surg. 2009; 135(6): 597-601. Wojciechowski B. Management of COPD exacerbations. Focus Journal. 2010; 22-23 and 35. www.uptodate.com
23
Potrebbero piacerti anche
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDa EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryValutazione: 3.5 su 5 stelle3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Da EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Valutazione: 4.5 su 5 stelle4.5/5 (119)
- MH Spartacus Workout PosterDocumento1 paginaMH Spartacus Workout PosterCindy100% (3)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDa EverandNever Split the Difference: Negotiating As If Your Life Depended On ItValutazione: 4.5 su 5 stelle4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDa EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaValutazione: 4.5 su 5 stelle4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingDa EverandThe Little Book of Hygge: Danish Secrets to Happy LivingValutazione: 3.5 su 5 stelle3.5/5 (399)
- Grit: The Power of Passion and PerseveranceDa EverandGrit: The Power of Passion and PerseveranceValutazione: 4 su 5 stelle4/5 (587)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDa EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyValutazione: 3.5 su 5 stelle3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDa EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeValutazione: 4 su 5 stelle4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnDa EverandTeam of Rivals: The Political Genius of Abraham LincolnValutazione: 4.5 su 5 stelle4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeDa EverandShoe Dog: A Memoir by the Creator of NikeValutazione: 4.5 su 5 stelle4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerDa EverandThe Emperor of All Maladies: A Biography of CancerValutazione: 4.5 su 5 stelle4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDa EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreValutazione: 4 su 5 stelle4/5 (1090)
- Her Body and Other Parties: StoriesDa EverandHer Body and Other Parties: StoriesValutazione: 4 su 5 stelle4/5 (821)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDa EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersValutazione: 4.5 su 5 stelle4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDa EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceValutazione: 4 su 5 stelle4/5 (890)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDa EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureValutazione: 4.5 su 5 stelle4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaDa EverandThe Unwinding: An Inner History of the New AmericaValutazione: 4 su 5 stelle4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)Da EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Valutazione: 4 su 5 stelle4/5 (98)
- Advanced SQL Functions in Oracle 10gDocumento417 pagineAdvanced SQL Functions in Oracle 10gYumiingNessuna valutazione finora
- On Fire: The (Burning) Case for a Green New DealDa EverandOn Fire: The (Burning) Case for a Green New DealValutazione: 4 su 5 stelle4/5 (73)
- Samsung Camera S630 / S730 User ManualDocumento98 pagineSamsung Camera S630 / S730 User ManualSamsung CameraNessuna valutazione finora
- The AMBOSS 100 Day Study Plan - Your No1 Study Guide For Final ExamsDocumento30 pagineThe AMBOSS 100 Day Study Plan - Your No1 Study Guide For Final Examsovermega100% (1)
- 7 Steps To Find Soulmate EbookDocumento50 pagine7 Steps To Find Soulmate EbookCindy100% (1)
- 7 Steps To Find Soulmate EbookDocumento50 pagine7 Steps To Find Soulmate EbookCindy100% (1)
- 7 Steps To Find Soulmate EbookDocumento50 pagine7 Steps To Find Soulmate EbookCindy100% (1)
- 7 Steps To Find Soulmate EbookDocumento50 pagine7 Steps To Find Soulmate EbookCindy100% (1)
- Stroke RehabilitationDocumento43 pagineStroke RehabilitationHashini Vjkmr100% (4)
- Basics of Cycling TrainingDocumento19 pagineBasics of Cycling Trainingmodulofriki100% (4)
- Fall Prevention Using TelemonitoringDocumento14 pagineFall Prevention Using Telemonitoringapi-458433381Nessuna valutazione finora
- Qbase Medicine 1 MCQs For The MRCPDocumento132 pagineQbase Medicine 1 MCQs For The MRCPsosoposo2100% (2)
- MH Jan06 PosterDocumento2 pagineMH Jan06 PosterCindy100% (1)
- Seminar On Minor Ailments and Complications of PuerperiumDocumento74 pagineSeminar On Minor Ailments and Complications of PuerperiumKaruna Kumari89% (46)
- Hospital DocumentsDocumento17 pagineHospital DocumentsRaviraj PisheNessuna valutazione finora
- Physiotherapy Guide for Respiratory & Cardiac Issues in Adults & ChildrenDocumento1 paginaPhysiotherapy Guide for Respiratory & Cardiac Issues in Adults & ChildrenAndrei Briceag100% (1)
- A History of The Canadian DollarDocumento119 pagineA History of The Canadian Dollarmintcorner100% (1)
- A History of The Canadian DollarDocumento119 pagineA History of The Canadian Dollarmintcorner100% (1)
- Answer Key EXAM DRILL 1 - Community Health Nursing Nursing Practice Ii - CHN and Care of The Mother and ChildDocumento11 pagineAnswer Key EXAM DRILL 1 - Community Health Nursing Nursing Practice Ii - CHN and Care of The Mother and Childbetiful100% (5)
- Consensus On The Pre-Hospital Approach To BurnsDocumento5 pagineConsensus On The Pre-Hospital Approach To BurnsCindyNessuna valutazione finora
- Fundamentals of Electric Propulsion Ion and Hall ThrustersDocumento8 pagineFundamentals of Electric Propulsion Ion and Hall ThrustersCindy0% (1)
- Consensus On The Pre-Hospital Approach To BurnsDocumento5 pagineConsensus On The Pre-Hospital Approach To BurnsCindyNessuna valutazione finora
- KariWilliams ManagementHospitalizedDocumento23 pagineKariWilliams ManagementHospitalizedCindyNessuna valutazione finora
- Mens Health - Break Thru Nutrition PlanDocumento26 pagineMens Health - Break Thru Nutrition PlanDavid PazdenNessuna valutazione finora
- Fundamentals of Electric Propulsion Ion and Hall ThrustersDocumento8 pagineFundamentals of Electric Propulsion Ion and Hall ThrustersCindy0% (1)
- The Science of Thinking - Europe Next IdeasDocumento36 pagineThe Science of Thinking - Europe Next IdeasCindyNessuna valutazione finora
- Power NutritionDocumento6 paginePower NutritionCindyNessuna valutazione finora
- Power NutritionDocumento6 paginePower NutritionCindyNessuna valutazione finora
- Sexual Selection and Genital EvolutionDocumento7 pagineSexual Selection and Genital EvolutionCindyNessuna valutazione finora
- SAS Intelligence Platform Overview Second EditionDocumento57 pagineSAS Intelligence Platform Overview Second EditionCindyNessuna valutazione finora
- 2008 Sant Language of SuccessDocumento68 pagine2008 Sant Language of SuccessCindyNessuna valutazione finora
- The Evolution of Female Mate Choice by Sexual Con FiDocumento9 pagineThe Evolution of Female Mate Choice by Sexual Con FiCindyNessuna valutazione finora
- Digital SLR Comparison Chart: D3X D3S D700 D300S D7000 D90 D5000 D3100 D3000Documento4 pagineDigital SLR Comparison Chart: D3X D3S D700 D300S D7000 D90 D5000 D3100 D3000Danielle FarhatNessuna valutazione finora
- Proc SQL V Data StepDocumento35 pagineProc SQL V Data StepCindyNessuna valutazione finora
- 4.3.1 Triage in Light of Four Hour TargetDocumento16 pagine4.3.1 Triage in Light of Four Hour TargetWilliam Wagner Müller XavierNessuna valutazione finora
- NURSING PRACTICE 3 Edited AnswerkeyDocumento9 pagineNURSING PRACTICE 3 Edited Answerkeykim_liñanNessuna valutazione finora
- BSU-CON Case Study on Breast Cancer Stage IIIBDocumento106 pagineBSU-CON Case Study on Breast Cancer Stage IIIBfLOR_ZIANE_MAENessuna valutazione finora
- The Significant Association Between Maternity Waiting Homes Utilization and Perinatal Mortality in Africa: Systematic Review and Meta-AnalysisDocumento6 pagineThe Significant Association Between Maternity Waiting Homes Utilization and Perinatal Mortality in Africa: Systematic Review and Meta-AnalysisTegenne LegesseNessuna valutazione finora
- Addis Ababa Sciece and Technology University Collage of Biological and Chemical Engineering Department of BiotechnologyDocumento14 pagineAddis Ababa Sciece and Technology University Collage of Biological and Chemical Engineering Department of BiotechnologyEshetu ShemetNessuna valutazione finora
- Dr. H. Pernodjo Dahlan SP.S (K)Documento20 pagineDr. H. Pernodjo Dahlan SP.S (K)hhamiemNessuna valutazione finora
- DBM-DOH jc2022-0002Documento18 pagineDBM-DOH jc2022-0002Drop ThatNessuna valutazione finora
- Community Case Serhat KokenDocumento12 pagineCommunity Case Serhat Kokenmaroun ghalebNessuna valutazione finora
- TB Drug StudyDocumento15 pagineTB Drug StudyKaloy KamaoNessuna valutazione finora
- Sample Legal Letter of Notice To Principles and School NursesDocumento2 pagineSample Legal Letter of Notice To Principles and School NursesJimUKNessuna valutazione finora
- Endo Logbook FormsDocumento3 pagineEndo Logbook FormsAmethystVonNessuna valutazione finora
- Principles of Bag TechniqueDocumento3 paginePrinciples of Bag TechniqueClare AlcoberNessuna valutazione finora
- B-2211 Implementation of DCI Revised B.D.S. CourseDocumento17 pagineB-2211 Implementation of DCI Revised B.D.S. CourseShital KiranNessuna valutazione finora
- S.S. Hospital OPD ScheduleDocumento4 pagineS.S. Hospital OPD Schedulegaurav SinghNessuna valutazione finora
- RCL Physical Exam Guidelines For Examining Physician 11-2014Documento4 pagineRCL Physical Exam Guidelines For Examining Physician 11-2014George Mihalache100% (1)
- Definition of TermsDocumento2 pagineDefinition of TermsjennahNessuna valutazione finora
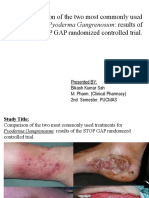
- Pyoderma GangrenosumDocumento18 paginePyoderma GangrenosumBikash SahNessuna valutazione finora
- Impact of Topical Steroids on Acanthamoeba Keratitis OutcomesDocumento8 pagineImpact of Topical Steroids on Acanthamoeba Keratitis OutcomesDiana BaagilNessuna valutazione finora
- Nonconventional Formocresol Pulpotomy Saves Tooth StructureDocumento6 pagineNonconventional Formocresol Pulpotomy Saves Tooth StructureMayerNessuna valutazione finora
- The Tuskegee Syphilis Experiment: Carolinak12@Unc - EduDocumento12 pagineThe Tuskegee Syphilis Experiment: Carolinak12@Unc - EdufirdausNessuna valutazione finora
- Fist Ulog RamDocumento5 pagineFist Ulog Ramansmart997373Nessuna valutazione finora
- Nursing Informatics 453X Assessment 1 Foundations of HealthDocumento3 pagineNursing Informatics 453X Assessment 1 Foundations of Healthjames mwangiNessuna valutazione finora